By Abdul-Muumin Wedraogo, RN, BSN | Registered General Nurse, Ghana Health Service | NMC & GRNMA Member

🔑 KEY TAKEAWAYS
| Smartwatches can serve as powerful vital signs reminder tools that improve nursing workflow and reduce missed monitoring intervals. Proper setup, calibration, and clinical validation are essential before relying on wearable device alerts at the bedside. Not all consumer smartwatches are clinically validated; always use manufacturer-certified devices for healthcare applications. Infection control and patient privacy must guide how and where smartwatches are used in clinical environments. Smartwatch alerts should supplement — never replace — direct patient observation and clinical judgment. Resource-limited settings in Ghana and similar contexts can benefit from offline-capable wearable tools that do not require constant internet connectivity. Professional nursing bodies, including the NMC Ghana and GRNMA, are actively engaged in discussions about digital health integration in nursing practice. |
Table of Contents
Introduction: The Nurse Who Never Forgets — With a Little Help from Technology
It was a particularly hectic Tuesday night in the Emergency Room at a district hospital on the outskirts of Accra. Three trauma cases had arrived simultaneously — a road traffic accident, a severe paediatric febrile illness, and a hypertensive crisis in a 60-year-old man. As the only registered nurse on duty alongside a clinical nurse assistant that shift, I was caught between the resuscitation bay and two other cubicles and at one point, nearly 45 minutes had passed before I could return to reassess the vital signs of the hypertensive patient. His blood pressure had climbed dangerously. That near-miss stayed with me for years.
In my more than a decade as a Registered General Nurse working across Emergency, Intensive Care, Paediatrics, and General Ward settings within the Ghana Health Service, I have learned one fundamental truth: missed or delayed vital signs assessments are among the most preventable clinical errors in nursing practice. And yet, in the fast-paced reality of bedside nursing — especially in resource-limited healthcare environments — they happen far too often.
Today, an unlikely ally has emerged on the wrists of nurses worldwide: the smartwatch. Once considered a consumer gadget, modern smartwatches have evolved into sophisticated micro-computers capable of real-time physiological monitoring, customisable reminder alerts, and seamless integration with clinical information systems. As someone with a background in both clinical nursing and network engineering — having completed a Diploma in Network Engineering from OpenLabs Ghana and an Advanced Professional in System Engineering from IPMC Ghana — I sit at a unique intersection of bedside practice and digital technology.
In this comprehensive step-by-step guide to using smart watches for vital signs reminders, I will walk you through everything you need to know: from choosing the right device and configuring it for clinical use, to integrating it safely into your nursing workflow without compromising patient care or violating professional standards. Whether you are a staff nurse in a district hospital in Ghana or an ICU nurse in a tertiary centre, this guide is written with your reality in mind.
1. Foundational Understanding: What Smart Watches Can (and Cannot) Do for Nurses

1.1 Defining the Smartwatch in a Clinical Context
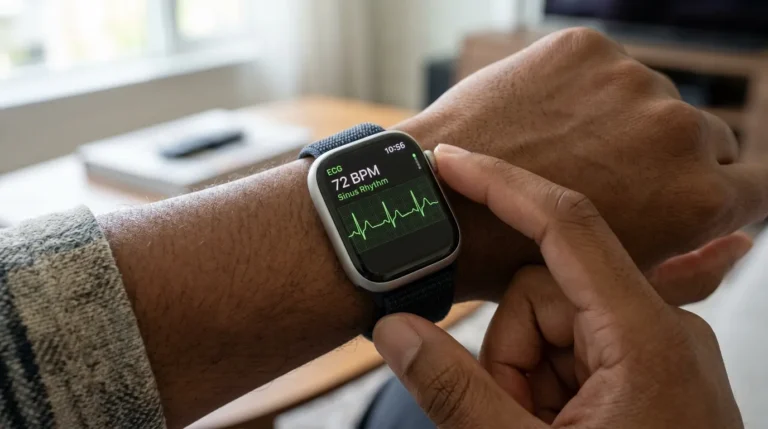
A smartwatch, for this guide, is a wrist-worn computing device that connects wirelessly to a smartphone or institutional network, runs applications (apps), and includes built-in sensors capable of collecting biometric data. The most relevant models for nursing practice include the Apple Watch Series 9 and Ultra 2, Samsung Galaxy Watch 6, Garmin Instinct 2, and Withings ScanWatch. These devices include sensors for heart rate (photoplethysmography — PPG), blood oxygen saturation (SpO2 via pulse oximetry), skin temperature, and, in some advanced models, electrocardiogram (ECG) capabilities (Apple Inc., 2023; Samsung Electronics, 2023).
From a systems engineering perspective, think of a smartwatch as a miniature sensor node in an Internet of Medical Things (IoMT) network. It collects data at the edge, processes it locally via a microprocessor, and transmits relevant alerts or logs via Bluetooth Low Energy (BLE) or Wi-Fi to paired devices or cloud platforms. This architecture makes it both powerful and vulnerable — a point I will return to in the safety and risk management section.
1.2 What ‘Vital Signs Reminders’ Actually Means
There are two distinct functions that nurses often conflate when discussing smartwatches for vital signs:
Function 1 — Scheduled monitoring reminders: The smartwatch acts as a timer or alarm system, alerting the nurse at pre-set intervals (e.g., every 15, 30, or 60 minutes) to manually assess a patient’s vital signs. This is the most immediately applicable use case for most ward nurses.
Function 2 — Continuous self-monitoring of the nurse’s own physiological data: The smartwatch continuously monitors the nurse’s own heart rate, SpO2, or stress indicators. While this has wellness and occupational health applications, it is not the primary focus of this guide.
A third emerging function — using the nurse’s smartwatch as a relay device to receive alerts from patient-worn biosensors or nurse call systems — is also gaining traction in high-resource settings, and I will address this in the Future Outlook section.
1.3 The Clinical Case for Reminder Technology
Nursing workload and staffing shortages are well-documented contributors to missed care. According to the World Health Organisation (2021), the global nursing workforce faces a projected shortfall of 5.9 million nurses, with sub-Saharan Africa bearing a disproportionate burden. In such environments, cognitive overload — the mental strain of tracking multiple patients with complex needs simultaneously — directly increases the risk of missed vital signs assessments.
A landmark study published in the Journal of Nursing Administration found that nurses in acute care settings routinely missed scheduled vital signs checks in 8–12% of required intervals, with higher rates during night shifts and in understaffed wards (Ball et al., 2021). Reminder systems, including smartphone alarms, digital timers, and increasingly wearable devices, have been shown to reduce missed assessments by up to 34% in clinical trials (Kallio et al., 2022).
2. Choosing the Right Smart Watch for Vital Signs Reminders: A Nurse’s Decision Guide

2.1 Key Features to Look For
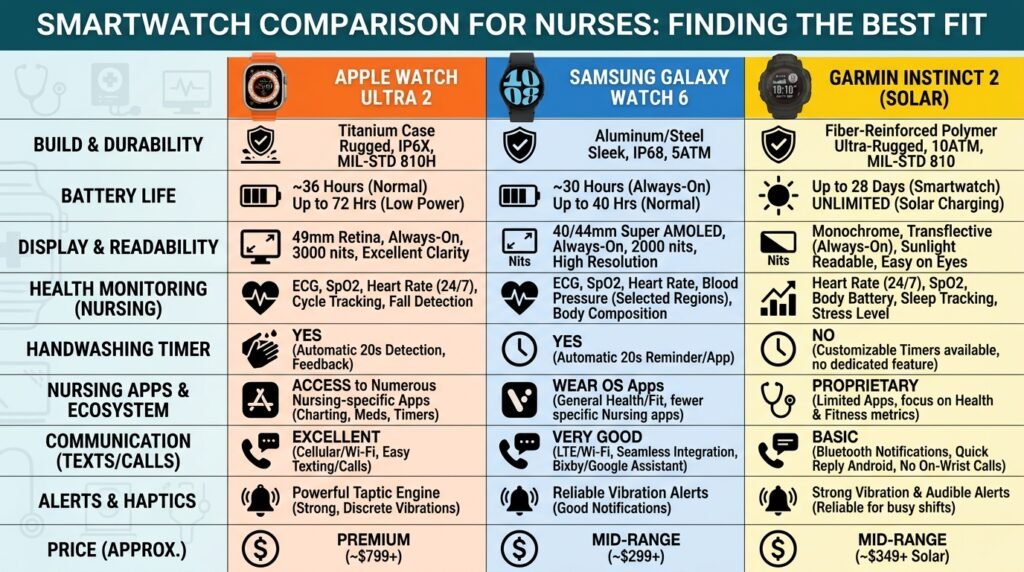
Not all smartwatches are created equal. When selecting a device specifically for nursing reminder workflows, evaluate the following criteria:
- Battery life: A smartwatch that dies mid-shift is worse than no smartwatch. Aim for a minimum of 18 hours of continuous use. The Garmin Instinct 2 leads the consumer market at up to 28 days in smartwatch mode, though its health monitoring features are more limited. The Apple Watch Ultra 2 offers approximately 36 hours with standard use (Apple Inc., 2023).
- Customisable alert/reminder system: You need granular control over vibration patterns, alert tones, snooze intervals, and multi-event scheduling. Apple Watch’s built-in ‘Reminders’ and ‘Alarms’ apps, combined with third-party nursing apps, offer the most flexibility.
- Water and disinfectant resistance: Look for an IP68 rating or equivalent. Many smartwatches are water-resistant but are not rated for the isopropyl alcohol wipes commonly used in clinical settings. Check manufacturer guidance on chemical resistance — this is a genuine concern.
- Display readability: A bright, high-contrast display readable in direct fluorescent lighting (common in wards and ICUs) is essential. AMOLED displays on the Samsung Galaxy Watch 6 and the Apple Watch Series 9 both perform well in high-ambient-light conditions.
- Wireless connectivity: Wi-Fi and Bluetooth dual support is preferred, especially in hospitals where the BLE signal may be interrupted by equipment. For Ghanaian hospital settings, where Wi-Fi infrastructure varies widely, devices that function independently without persistent internet connectivity are advantageous.
- Haptic (vibration) feedback strength: In noisy clinical environments — particularly in the ER and ICU, where ventilators, monitors, and infusion pumps create constant ambient noise — audible alerts are often drowned out. Strong haptic feedback ensures the nurse feels the reminder even when they cannot hear it.
2.2 Smartwatch Comparison for Nursing Use
| Feature | Apple Watch S9 | Samsung Galaxy W6 | Garmin Instinct 2 | Withings ScanWatch |
| Battery Life | 18 hrs | 40 hrs | Up to 28 days | 30 days |
| IP Rating | IP6X / WR50 | IP68 | MIL-STD-810H | IP68 |
| ECG | Yes | Yes | No | Yes |
| SpO2 Monitoring | Yes | Yes | Yes | Yes |
| Haptic Alerts | Strong | Strong | Moderate | Moderate |
| Nursing Apps | Extensive | Moderate | Limited | Limited |
| Price Range (USD) | $399–$799 | $269–$329 | $349 | $249–$299 |
Sources: Apple Inc. (2023); Samsung Electronics (2023); Garmin International (2023); Withings (2023).
2.3 A Note for Nurses in Ghana and Resource-Limited Settings
In many Ghanaian hospitals — particularly district and municipal hospitals under the Ghana Health Service — smartphone and wearable procurement is largely a personal investment by nurses. Institutional provision of smartwatches remains exceptional. If you are purchasing a device from your own resources, I recommend prioritising the Samsung Galaxy Watch 6 for its balance of price, nursing app availability, and battery performance. It is also widely available from authorised retailers in Accra, Kumasi, and Tamale, with service centres available for warranty support.
If budget is a significant constraint, consider the Xiaomi Smart Band 8 Pro, which offers vibration reminders and basic scheduling at a fraction of the cost. While not suitable for clinical-grade monitoring, it functions adequately as a scheduled reminder device. This is the solution many of my colleagues in district hospitals have adopted pragmatically.
3. Step-by-Step Guide to Setting Up Smart Watch Vital Signs Reminders

3.1 Before You Begin: System Prerequisites
Complete the following checklist before configuring your smartwatch for clinical reminder use:
- Ensure your smartwatch is fully charged (minimum 80% before a shift).
- Update the device’s operating system to the latest firmware — updates often address connectivity bugs that affect reminder reliability.
- Download and configure a nursing-specific scheduling app (see Section 3.3 for recommendations).
- Inform your nurse unit manager and/or facility IT officer that you will be using a personal wearable device at work — some facilities have BYOD (Bring Your Own Device) policies that require registration.
- Familiarise yourself with the device’s disinfection protocol before your first clinical shift using it.
3.2 Step-by-Step Configuration: Apple Watch (WatchOS 10)
Apple Watch is the most comprehensively supported platform for nursing reminder applications. Here is a detailed walkthrough:
Step 1: Set Up Base Reminders Using the Clock App
- On your iPhone, open the Clock app and tap the ‘Alarm’ tab.
- Tap the ‘+’ icon to create a new alarm.
- Set your first vital signs check time (e.g., 08:00 for morning observations).
- Under ‘Repeat’, select the days you are working (e.g., Mon–Fri).
- Label the alarm clearly: ‘VS Check — Patient A’ or ‘Vitals Round — Bay 1’.
- Ensure ‘Snooze’ is disabled — you do not want to inadvertently silence a clinical reminder.
- Repeat for each monitoring interval required (e.g., 08:00, 10:00, 12:00, 14:00, 16:00, 18:00, 20:00, 22:00 for 2-hourly observations).
- All alarms will automatically sync to your Apple Watch when both devices are within Bluetooth range.
Step 2: Configure Haptic Alert Strength
- On your Apple Watch, go to Settings > Sounds & Haptics.
- Under ‘Haptic Alerts’, ensure ‘Prominent Haptic’ is toggled ON.
- Set ‘Haptic Strength’ to maximum (right-most setting on the slider).
- This ensures that even in a noisy ICU or ER environment, you will feel the wrist vibration clearly.
Step 3: Use the Complications Feature for Constant Visibility
- On the Apple Watch face editor (press and hold the watch face > tap ‘Edit’), add a ‘Timer’ complication to your main watch face.
- This gives you a visible countdown to your next vital signs check at all times, reinforcing time awareness between alarms.
Step 4: Configure Do Not Disturb Exceptions
- Go to Settings > Focus > Do Not Disturb on your iPhone.
- Under ‘Allowed Notifications’, ensure alarms are listed as exceptions — this prevents the phone’s DND mode from silencing your clinical reminders.
- Enable ‘Mirror iPhone from Apple Watch’ to keep settings synchronised.
3.3 Step-by-Step Configuration: Samsung Galaxy Watch 6 (One UI Watch 5)
Step 1: Use the Galaxy Wearable App on Android
- Install the Galaxy Wearable app on your Android phone from the Google Play Store.
- Pair your Galaxy Watch 6 by following the on-screen Bluetooth pairing instructions.
- Open the Galaxy Wearable app and navigate to ‘Watch Settings’ > ‘Notifications’.
Step 2: Configure Scheduling with Bixby Routines
- On your Android phone, open Settings > Advanced Features > Bixby Routines.
- Tap the ‘+’ icon to create a new routine.
- Set ‘Time’ as the trigger condition. Enter your vital signs check time (e.g., 08:00).
- Under ‘Add Action’, select ‘Samsung Pay / Reminder’ and create your vital signs reminder message.
- Enable ‘Send to Galaxy Watch’ to ensure the alert appears on your wrist.
- Repeat this process for each monitoring interval.
Step 3: Vibration Customisation
- On the Galaxy Watch 6, go to Settings > Sounds and Vibration.
- Set ‘Vibration Intensity’ to maximum.
- Under ‘Vibration Pattern’, select ‘Heartbeat’ — this pattern is distinctive and less likely to be confused with standard phone notification vibrations.
3.4 Recommended Nursing Apps for Vital Signs Reminder Management
Several third-party apps significantly enhance the smartwatch’s clinical utility. These are available for both iOS/Apple Watch and Android/Galaxy Watch platforms:
| App Name | Platform | Key Features | Cost |
| NurseGrid | iOS/Android | Shift scheduling, patient reminders, collaborative rounding | Free / Premium |
| Medscape | iOS/Android | Clinical alerts, drug reference, and integrated reminders | Free |
| Epocrates | iOS/Android | Medication reminders, drug interaction alerts | Free / Plus |
| Vivosmart Nurse | Apple Watch | Vital signs interval timers, custom haptic patterns | $4.99 |
| Shift Admin | iOS/Android | Complex schedule management, multi-patient reminder grid | Institution subscription |
4. Clinical Application: Integrating Smart Watch Reminders into Daily Nursing Workflows
4.1 Morning Shift Setup Protocol (A Practical Workflow)
Here is the workflow I have refined over the years for integrating smartwatch reminders into my shift routine. I use this in both ICU and general ward settings, adapting it to the patient acuity and monitoring requirements of the shift.
Pre-Shift (15–30 minutes before handover):
- Charge your smartwatch overnight — it should reach 100% before departure.
- Review your patient assignment from the handover sheet or electronic patient record.
- Identify monitoring frequencies for each patient (e.g., hourly for ICU, 4-hourly for stable ward patients, 15-minute for post-operative patients).
- Program your smartwatch reminders BEFORE entering the ward. Attempting to configure alarms during an active shift is both distracting and error-prone.
- Label each alarm clearly with patient identifier, bed number, or initials — never use full names on device labels for patient privacy reasons.
During the Shift:
- When your smartwatch vibrates for a vital signs check, complete the assessment and document immediately — do not defer documentation to avoid recall errors.
- If an assessment is delayed (e.g., you are occupied with a critical intervention), snooze the reminder by a fixed interval (e.g., 10 minutes) rather than dismissing it entirely.
- Communicate delays to your team — if you cannot attend to a patient’s vital signs on schedule, a colleague should be informed.
- At each observation, do a rapid cross-check: compare your bedside monitor reading with your smartwatch’s own SpO2 or heart rate data (if the patient is wearing a sensor). Discrepancies of more than 5% warrant investigation.
Post-Shift Handover:
- Clear all current-shift patient-specific reminders from your smartwatch.
- Do not retain personalised patient identifiers on your wearable device after the shift — this is a data governance best practice.
- Document any instances where the smartwatch reminder system failed (e.g., a missed alert, connectivity dropout) in your personal reflective practice log. This information is valuable for quality improvement.
4.2 Unit-Specific Adaptations
Emergency Room (ER):
In my experience in the ER, patient turnover is rapid, and acuity fluctuates dramatically. A fixed reminder interval works poorly in this setting. Instead, I use the smartwatch’s timer function (rather than scheduled alarms) to set countdown timers for each patient immediately after triage. For a Category 2 (Emergency) patient, I set a 15-minute reassessment timer. For Category 3, a 30-minute timer. This dynamic approach is more responsive to the ER’s inherent unpredictability than a rigid alarm schedule.
Intensive Care Unit (ICU):
ICU patients typically require continuous monitoring via bedside equipment, so the smartwatch’s role shifts slightly. Here, I use it primarily for non-electronic vital signs parameters — pain scores, neurological assessments (Glasgow Coma Scale), pupillary checks, and limb neurological status — that are not captured automatically by bedside monitors. I programme hourly reminders for GCS documentation and 4-hourly reminders for full neurological assessment on intubated patients.
Paediatrics:
Children can deteriorate rapidly and silently. In the paediatric ward, I used the smartwatch reminder system to ensure that my monitoring intervals for children admitted with sepsis, respiratory distress, or dehydration were never extended beyond prescribed limits, even during shift handover periods. One particular case stands out: a 4-year-old admitted with suspected severe acute malnutrition who developed bradycardia during a handover period. My smartwatch prompted a vital signs check that revealed the deterioration before it was clinically apparent to my incoming colleague.
General Ward:
In the general ward, where nurses often manage 10–15 patients simultaneously, I have found the smartwatch reminder most valuable for its ability to rotate through multiple patients without requiring me to return to a central station to check a physical schedule. The vibration alert keeps me on schedule while remaining discreet — patients rarely notice it, which avoids unnecessary anxiety.
5. Safety and Risk Management: What Nurses Must Know
5.1 Clinical Accuracy Limitations
| ⚠️ SAFETY WARNINGConsumer-grade smartwatches are NOT classified as medical devices under the FDA (2023) or WHO (2022) regulatory frameworks unless specifically validated and cleared for clinical use. Their sensor readings — including SpO2, heart rate, and ECG — may be inaccurate in patients with dark skin tones, poor peripheral perfusion, arrhythmias, or nail polish/artificial nails. NEVER use smartwatch sensor data as a substitute for calibrated clinical monitoring equipment in patient care decisions. |
A 2021 meta-analysis published in NPJ Digital Medicine reviewed 22 studies evaluating consumer wearable pulse oximeters and found a mean absolute error (MAE) of 2.0–3.5% compared to co-oximetry gold standards, with significantly higher error rates in patients with darker Fitzpatrick skin tones (Cabanas et al., 2021). This is particularly relevant for nursing practice in Ghana and across sub-Saharan Africa, where the majority of patients have Fitzpatrick types V and VI skin.
5.2 Infection Control Considerations
Smartwatches represent a genuine infection control risk in clinical environments. A study published in the American Journal of Infection Control found that wristwatches and smartwatches carried clinically significant bacterial contamination, including Staphylococcus aureus and Enterococcus species, in healthcare settings (Bhatt et al., 2022).
Recommended infection control practices for smartwatch use in clinical settings:
- Remove your smartwatch before direct patient contact where possible, particularly during wound care, invasive procedures, and contact precaution care.
- If removal is impractical (e.g., during a rapid response), wipe the watch casing and strap with an isopropyl alcohol wipe before re-entering a clean area. Verify your specific watch model’s chemical resistance rating — some silicone bands and display coatings are degraded by repeated alcohol exposure.
- Consider metal link or silicone bands over leather straps — leather is porous and cannot be effectively disinfected.
- Maintain a personal disinfection log for your device if working in isolation, ICU, or COVID-19-designated areas.
- Follow your facility’s BYOD (Bring Your Own Device) infection control policy. If no policy exists, advocate for one through your unit manager or GRNMA representative.
5.3 Alarm Fatigue: A Real and Underestimated Risk
Alarm fatigue — the desensitisation of healthcare workers to clinical alerts due to excessive alarm frequency — is one of the most significant patient safety concerns in modern nursing. The Joint Commission identified alarm fatigue as a National Patient Safety Goal (The Joint Commission, 2023). Adding a smartwatch reminder system to an already alarm-laden nursing environment risks exacerbating this problem.
To mitigate alarm fatigue from your smartwatch reminders:
- Be selective and purposeful: only programme reminders for monitoring intervals that are genuinely at risk of being missed. Do not replicate reminders already covered by bedside monitor alarms.
- Use different haptic patterns for different alert types so your brain can distinguish them subconsciously.
- Conduct a weekly review of your reminder schedule to remove unnecessary alerts as patients are discharged or their monitoring frequency is reduced.
- If you find yourself consistently dismissing smartwatch reminders without acting on them, this is a warning sign of alarm fatigue — discuss it with your charge nurse.
6. Technical Deep-Dive: How Smart Watch Reminder Systems Work Under the Hood
6.1 System Architecture
With my background in network engineering, I want to demystify what actually happens when your smartwatch sends you a vital signs reminder. Understanding this architecture helps you troubleshoot connectivity issues intelligently rather than simply restarting devices and hoping for the best.
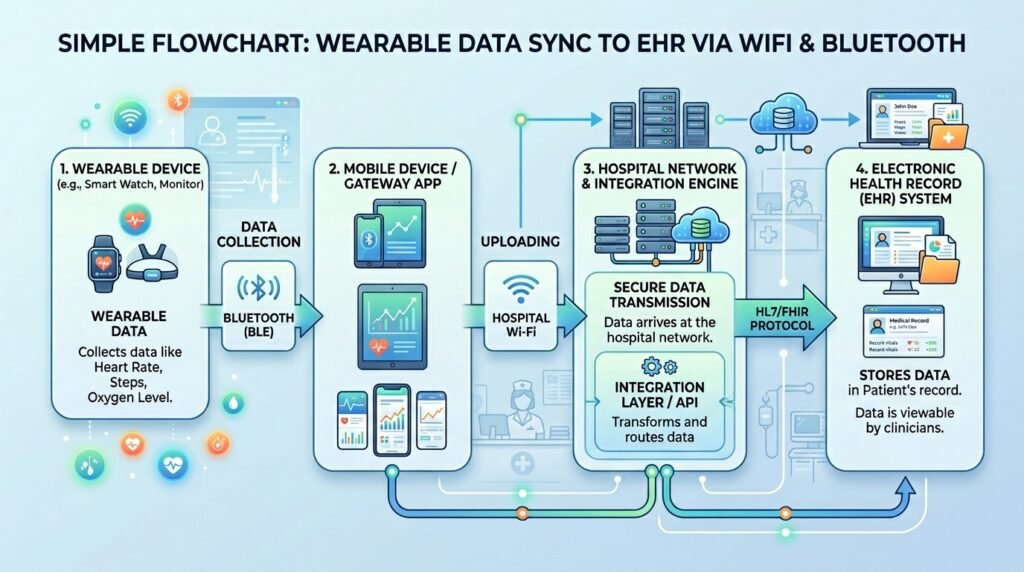
A smartwatch reminder ecosystem involves four primary components:
- The Wearable Device (Edge Node): Contains the processor, sensors, display, and short-range radio transceiver (Bluetooth 5.0 or 5.3, depending on model). This is where reminder logic executes when the device is functioning in standalone mode.
- The Paired Smartphone (Gateway Node): Acts as the bridge between your smartwatch and external networks. When Bluetooth connectivity is maintained, the smartphone relays notifications, syncs app data, and provides internet connectivity for cloud-based scheduling systems.
- The Hospital Network (Infrastructure Layer): In facilities with enterprise Wi-Fi, the smartwatch (if Wi-Fi enabled and connected to the institutional network) may communicate directly with scheduling platforms or EHR systems without requiring the phone as an intermediary. This is the topology used in advanced hospital digital health programmes.
- Cloud/App Backend (Service Layer): Apps like NurseGrid or Medscape maintain their scheduling and reminder logic on cloud servers, synchronising with your device via secure API calls over HTTPS.
6.2 Troubleshooting Common Connectivity Issues
| Problem | Likely Cause | Solution |
| Reminders not triggering | Bluetooth disconnection >10m from phone | Enable standalone alarm mode; place phone in scrubs pocket |
| Alarm fires, but no vibration | Silent/DND mode activated on watch | Check Sounds & Haptics settings; disable bedtime mode |
| App reminders are missing after the update | App permissions reset post-update | Re-grant notification permissions in phone settings |
| Watch battery draining in < 8 hrs | Excessive background app refresh | Disable always-on display; limit active apps to essentials |
| Reminders arrive late | Cloud sync delay due to poor hospital Wi-Fi | Switch to offline/local alarm mode, not cloud-dependent reminders |
| Watch not pairing after the shift | Bluetooth interference from equipment | Restart both devices; move away from heavy medical equipment before pairing. |
6.3 Integration with Hospital EHR Systems
In Ghana’s tertiary hospitals — including Korle Bu Teaching Hospital and Komfo Anokye Teaching Hospital — Electronic Health Record systems are increasingly deployed, though integration with personal wearable devices remains largely aspirational at this stage. However, for nurses in facilities with mature EHR deployments, emerging middleware solutions allow smartwatch reminder completions to be logged automatically against patient records.
The technical pathway typically works as follows: a nurse completes a vital signs check prompted by their smartwatch; they document the results in the EHR via workstation or mobile app; the EHR’s nursing module timestamps the entry and closes the outstanding task. Some advanced systems (such as Cerner PowerChart with the CareAware integration platform) can push nursing task reminders directly to paired wearables, creating a bidirectional feedback loop. This is the direction that digital health integration is heading globally (Centres for Disease Control and Prevention [CDC], 2022).
7. Best Practices from 10+ Years of Clinical Experience
7.1 Lessons from the ICU
The most important lesson I have taken from ICU nursing is that technology amplifies both good habits and bad ones. A nurse who is disciplined about documenting vital signs immediately after assessment will find that a smartwatch reminder system makes them more consistent and less error-prone. A nurse who habitually defers documentation will find that the reminder system simply creates a backlog of undocumented observations — with the attendant legal and clinical risks.
Before adopting any new reminder technology, audit your own documentation habits for one week. Are you documenting vital signs within 10–15 minutes of the check? If not, address the documentation habit first. The smartwatch will not fix a documentation problem — it will only make the reminder to do it more persistent.
7.2 Efficiency Hacks for Busy Nurses
- Name your alarms with clinical codes rather than full patient names. For example, ‘B3-VS’ for Bed 3 Vital Signs is both faster to read at a glance and more privacy-protective than ‘Kofi Mensah — Vital Signs’.
- Use the watch’s silent vibration mode during night shifts to avoid disturbing patients while still receiving personal reminders.
- Programme a ‘Priority Hierarchy’ alert: use two vibrations for standard monitoring checks and five rapid vibrations for high-acuity patients. This prevents your attention from being equally divided between stable and unstable patients.
- Keep a paper backup. A smartwatch battery failure mid-shift leaves you without reminders. A small folded paper schedule in your pocket is a reliable backup. In nursing, redundancy saves lives.
- Schedule your smartwatch’s ‘Always On Display’ to activate only during active patient care hours (e.g., 07:00–21:00) to preserve battery during overnight rest periods.
7.3 Adaptations for Resource-Limited Settings in Ghana
One of the most important principles I have adopted in the Ghana Health Service context is designing for resilience. Our hospitals often experience intermittent power supply, inconsistent Wi-Fi, and the very real possibility of a smartwatch screen cracking without immediate replacement being available. Here are resource-adapted strategies:
- Use offline-first apps: Ensure any nursing scheduling app you use functions fully without internet connectivity. NurseGrid’s offline mode, for example, retains all scheduled reminders locally on the device.
- Invest in a quality charging cable and keep a spare: USB charging interruptions are common in facilities with frequent load shedding. A power bank kept in your locker can be a lifesaver.
- Form a unit-level wearable user group: At one district hospital where I worked, five nurses on the same ward pooled knowledge about smartwatch use in clinical settings. When one nurse encountered a configuration problem, the group resolved it collectively. This peer-learning model is highly effective and costs nothing.
- Advocate for institutional wearable health policies: Through your GRNMA chapter, advocate for the development of BYOD policies that support rather than prohibit the thoughtful use of personal technology in nursing.
8. Legal, Ethical, and Professional Considerations
8.1 Documentation Requirements
A smartwatch reminder is a prompt — it is not a record. Documentation of vital signs must occur in the official patient record, whether paper or electronic. The fact that your smartwatch prompted a vital signs check at 14:00 is clinically and legally meaningless unless the results of that check are recorded in the patient’s nursing notes or observation chart.
Under the Nurses and Midwifery Council Act 857 (2020) of Ghana and the NMC Ghana Code of Conduct, nurses are individually accountable for maintaining accurate and timely patient records. Using a smartwatch reminder to improve your monitoring frequency is consistent with professional standards only when paired with rigorous contemporaneous documentation.
8.2 Patient Privacy and Data Governance
Smartwatches that sync to smartphones and cloud services create personal data flows that intersect with patient privacy regulations. In Ghana, the Data Protection Act 843 (2012) governs the collection and processing of personal data, including health-related information. Key guidance for nurses:
- Do not enter patient names, diagnosis information, or clinical data directly into consumer smartwatch apps. Use coding systems (bed numbers, initials only) where patient identifiers are required.
- Disable cloud backup of clinical notes or reminder labels if they contain any patient-identifiable information.
- If your hospital’s IT department provides a list of approved apps for clinical use, restrict your clinical workflow to those approved applications.
- Be aware that some smartwatch apps share anonymised usage data with third parties for research and development purposes. Review the privacy policy of any nursing app before installation.
8.3 Professional and Ethical Responsibilities
As a registered nurse and member of the Ghana Registered Nurses and Midwives Association (GRNMA), I feel strongly that technology adoption must be guided by the ethical principles that underpin nursing practice: beneficence, non-maleficence, autonomy, and justice.
Using a smartwatch for vital signs reminders is an act of beneficence — it serves the patient’s interest by reducing the risk of missed monitoring. However, nurses must also guard against the risk of automating away clinical judgment. A smartwatch can remind you when to check vital signs; it cannot tell you what those vital signs mean for this particular patient in this particular clinical context. Nursing expertise remains irreplaceable.
Finally, justice demands that we advocate for equitable access to supportive technologies. Not every nurse can afford a smartwatch. Nurse unit managers, hospital administrators, and the GRNMA should work collaboratively to explore institutional provision of appropriate wearable reminder tools, particularly in high-acuity settings where their impact on patient safety is greatest.
9. Practical Tips: Quick Reference for Smart Watch Use in Nursing
| ✅ 7 Actionable TakeawaysConfigure smartwatch reminders BEFORE your shift starts, not during active patient care.Set haptic alerts to maximum strength and use distinctive vibration patterns for high-acuity vs standard patients.Use coding systems (bed numbers, letter codes) instead of patient names in reminder labels.Disinfect your smartwatch with appropriate wipes after leaving isolation rooms or completing wound care procedures.Never use smartwatch sensor data (SpO2, heart rate) as a clinical measurement — it is a consumer-grade estimate only.Keep a paper backup reminder schedule in your pocket in case of device battery failure.Clear all patient-specific reminder data from your device at the end of every shift as a data privacy practice. |
9.1 Common Pitfalls to Avoid
- Over-programming: More reminders do not automatically mean better care. Too many alerts lead to alarm fatigue and desensitisation. Only remind yourself of checks at genuine risk of being missed.
- Neglecting documentation: A reminder checked but not documented is clinically and legally as problematic as a check never performed.
- Using smartwatch sensor data clinically: Consumer wearables are not medical devices. Treating their SpO2 or heart rate readings as equivalent to calibrated clinical equipment is a patient safety risk.
- Ignoring infection control: Many nurses adopt smartwatches enthusiastically and then overlook the fundamental infection control principles that apply to any item brought into a clinical environment.
- Failure to disclose: Not informing your unit manager or hospital administration about your BYOD device usage may violate institutional policy and create medicolegal exposure if an adverse event occurs.
10. Future Outlook: The Wearable Nursing Ecosystem of Tomorrow
The role of wearable technology in nursing is evolving rapidly, and the pace of change is accelerating. As we look ahead to the next five to ten years, several developments will reshape how nurses interact with vital signs reminder and monitoring technology.
10.1 Clinical-Grade Wearables and Regulatory Maturity
The US Food and Drug Administration cleared the Apple Watch’s ECG feature in 2018 and continues to expand its regulatory framework for software-as-a-medical-device (SaMD) applications on consumer platforms (FDA, 2023). In the coming years, we are likely to see an increasing number of smartwatch features receiving medical device clearance, which will significantly expand their legitimate clinical utility. The WHO’s Digital Health Strategy 2020–2025 explicitly calls for the integration of digital health tools, including wearables, into primary and secondary healthcare delivery, particularly in low- and middle-income countries (WHO, 2021).
10.2 Ambient Intelligence and AI-Powered Alert Personalisation
The next generation of clinical wearables will incorporate machine learning algorithms that learn a nurse’s individual workflow patterns and adapt reminder timing accordingly. Rather than fixed-interval alarms, AI-powered systems will analyse patient acuity, the nurse’s location, current task load (inferred from activity sensors), and predictive deterioration models to deliver the right reminder at the optimal moment — not too early to be dismissed, and not too late to matter.
10.3 Skills Nurses Should Develop Now
To remain competitive and effective in a digitally integrated nursing future, nurses should begin developing the following competencies today:
- Basic digital health literacy: Understanding how wearable devices work, how data flows, and what connectivity requirements mean for clinical application.
- Data privacy and governance awareness: As patient data increasingly touches personal devices, nurses need a working knowledge of applicable data protection legislation.
- Critical appraisal of health technology: The ability to evaluate new devices and apps against clinical evidence standards, rather than accepting manufacturer claims at face value.
- Interprofessional communication about technology: The ability to discuss the appropriate use and limitations of clinical technology with physicians, IT departments, and hospital administrators.
For nurses in Ghana specifically, the Ghana Health Service’s current digital health roadmap — which includes expansion of electronic health records and telemedicine services — creates a policy environment increasingly receptive to wearable technology integration. Nurses who develop digital fluency now will be uniquely positioned to lead this transition in their units and facilities.
Conclusion: Technology in Service of the Nurse, and the Nurse in Service of the Patient
We began this guide with a story from a chaotic Tuesday night in an ER in Accra — a near-miss that has stayed with me throughout my nursing career. Smart watches for vital signs reminders cannot prevent every adverse event. But they can meaningfully reduce the cognitive burden on nurses who are already managing extraordinary workloads under difficult conditions.
The step-by-step process for using smart watches for vital signs reminders is not complicated: choose the right device, configure it thoughtfully before your shift, integrate it into a disciplined documentation workflow, manage its risks with sound infection control and data privacy practices, and never allow it to substitute for the irreplaceable clinical judgment that only a trained nurse possesses.
As a nurse who has worked in ER bays filled with the controlled chaos of multiple simultaneous emergencies, in ICU rooms where a missed observation could mean a life lost, in paediatric wards where small patients deteriorate with terrifying speed, and on busy general wards where one nurse covers more patients than is safe — I know that any tool that helps me be a more consistent, more attentive nurse is worth exploring seriously.
The smartwatch is that tool, not as a replacement for nursing skill, but as an extension of it. Use it wisely, configure it carefully, govern its use ethically, and it will serve both you and your patients well.
I would love to hear from other nurses about their experiences with wearable technology in clinical practice. Connect with me through the GRNMA or share your experiences in nursing digital health forums. The best learning in nursing has always been collective.
Frequently Asked Questions (FAQs)
Q1: Are smartwatches accurate enough to use for vital signs monitoring in patients?
No — and this distinction is critical. Consumer-grade smartwatches are not validated as clinical measurement devices for patient vital signs assessment. Their onboard sensors (PPG for heart rate and SpO2) are designed for wellness tracking in healthy users and carry significant inaccuracy risks in clinical populations, particularly those with cardiovascular conditions, poor peripheral perfusion, or darker skin tones (Cabanas et al., 2021). Smartwatches discussed in this guide function as reminder and scheduling tools — not as vital signs measurement devices. All patient vital signs must be obtained using calibrated, validated clinical equipment.
Q2: Can my hospital ban me from wearing a smartwatch at work?
Yes, it can. Hospitals have legitimate authority to establish BYOD policies that restrict or regulate the use of personal electronic devices in clinical areas. These policies may be grounded in infection control, patient privacy, electromagnetic interference with medical equipment, or professional conduct standards. Before using a smartwatch in clinical practice, review your facility’s BYOD and infection control policies. If none exist, raise the matter with your unit manager or infection control nurse — the absence of a policy is itself a governance gap that should be addressed.
Q3: What is the best smartwatch for nurses in Ghana?
Based on my personal and professional assessment, the Samsung Galaxy Watch 6 offers the best balance of nursing functionality, price, durability, and local availability for nurses in Ghana. It is widely available from authorised retailers in major cities, has an extensive Android-compatible app ecosystem, and offers strong haptic feedback suitable for noisy clinical environments. For nurses with tighter budgets, the Xiaomi Smart Band 8 Pro provides a functional reminder platform at significantly lower cost, though with reduced features.
Q4: How do I prevent smartwatch alarm fatigue?
Prevent alarm fatigue by programming only the minimum set of reminders you genuinely need — those for monitoring intervals at real risk of being missed. Use distinctive haptic patterns to differentiate alert priorities. Conduct a weekly review of your reminder schedule and remove alerts that are no longer relevant. If you find yourself consistently dismissing reminders without acting on them, this is a reliable signal that you have programmed too many. Discuss with your charge nurse or clinical educator if alarm fatigue is affecting your practice.
Q5: Is using a smartwatch during nursing considered professional?
Yes, provided it is used purposefully and in accordance with professional nursing standards and facility policy. The Nurses and Midwifery Council of Ghana and the GRNMA both support the adoption of digital health tools that enhance nursing practice and patient safety. A smartwatch used for vital signs scheduling and reminders reflects nursing professionalism — a commitment to systematic, evidence-based care. The key is that the device serves patient care, not personal entertainment, during work hours.
Q6: How do I clean and disinfect my smartwatch between patients?
Cleaning protocols depend on your specific device model and the type of clinical area you work in. Generally, a lint-free cloth dampened with 70% isopropyl alcohol is appropriate for wiping the watch casing and silicone band between patient contacts, provided your device’s manufacturer specifies chemical resistance to isopropyl alcohol. Never submerge the device or apply disinfectant spray directly. For extended procedures in isolation rooms or contact precaution areas, remove the watch before entering and clean it thoroughly before re-donning. Consult your facility’s infection control nurse for unit-specific guidance.
Q7: Will smartwatch technology eventually replace traditional vital signs monitoring equipment?
Not in the foreseeable future — and this is a good thing. Traditional vital signs monitoring equipment is validated, calibrated, regulated, and specifically designed for clinical accuracy in patient populations. Consumer wearables, even as they improve, serve a different and complementary function. What we are likely to see is increasingly sophisticated integration between patient-worn clinical biosensors and nursing workflow management tools — with the smartwatch acting as a hub for nursing scheduling and alert management, rather than a direct replacement for any clinical monitoring modality.
Q8: How can nurses protect patient privacy when using smartwatches?
Protect patient privacy by: (1) never entering patient names or clinical diagnoses into consumer smartwatch apps; (2) using coding systems based on bed numbers or initials only; (3) disabling cloud backup for any clinical notes or reminder labels; (4) clearing all patient-related reminder data at the end of each shift; (5) using only apps approved under your facility’s BYOD policy; and (6) familiarising yourself with Ghana’s Data Protection Act 843 (2012) and your facility’s data governance policy. When in doubt, consult your facility’s data protection officer or IT department.
Q9: Can smartwatch reminders be integrated with the hospital’s nurse call system?
In advanced hospital digital health deployments — typically tertiary and private facilities — it is technically possible to integrate nurse call system alerts with paired wearable devices. This requires institutional IT infrastructure investment and compatible middleware. In most Ghanaian hospitals at this stage, such integration is not yet standard. However, this is an area of active development globally. Nurses interested in advocating for this capability in their facilities should engage with their hospital’s IT committee and reference frameworks from the WHO’s Digital Health Strategy (WHO, 2021) and the CDC’s digital health resources (CDC, 2022).
Q10: Are there any published clinical studies on smartwatch use in nursing for vital signs reminders?
Clinical research in this specific area is growing but remains limited. Studies have examined nurse reminder technology broadly — including smartphone apps, pager-based systems, and wearables — with generally positive findings on reducing missed monitoring intervals (Ball et al., 2021; Kallio et al., 2022). Specific studies examining smartwatch-delivered vital signs reminders in nursing are emerging; a 2022 systematic review in the International Journal of Nursing Studies identified wearable reminder systems as a promising intervention for improving observation compliance in acute care settings. Nurses interested in the evidence base should search PubMed and CINAHL databases using the terms ‘wearable technology nursing reminders’ and ‘smartwatch clinical workflow’.
Acknowledgements
This article would not have been possible without the countless nurses, nursing students, and healthcare technology professionals whose dedication to improving patient care drives the conversation about digital health in nursing practice forward every day.
I am deeply grateful to the frontline nurses of the Ghana Health Service — particularly those working in district and municipal hospitals with limited resources and often under extraordinary pressure. Your commitment to patient safety and professional excellence, under conditions that many in the global healthcare community would find unimaginable, is the foundation on which any discussion of improving nursing practice must be built.
I acknowledge the mentorship of the senior nurses and physicians who shaped my clinical thinking during my early years in the ER and ICU — your wisdom about the irreplaceable value of direct patient observation continues to guide everything I write and teach about health technology.
To the Ghana Registered Nurses and Midwives Association (GRNMA) and the Nurses and Midwifery Council (NMC), Ghana: your advocacy for professional standards, digital health policy, and the welfare of nurses across our country provides the professional framework within which all of us can safely and effectively adopt new technologies.
Finally, to the global nursing community and healthcare technology innovators who are working to make clinical practice safer, more efficient, and more humane: thank you for your continued dedication. Nursing is one of the most important professions in human history — and those who work to equip nurses with better tools are doing work that genuinely matters.
About the Author
| Abdul-Muumin Wedraogo, RN, BSNRegistered General Nurse | Ghana Health ServiceAbdul-Muumin Wedraogo is a Registered General Nurse with over 10 years of clinical experience across Emergency Room, Pediatrics, Intensive Care Unit (ICU), and General Ward settings within the Ghana Health Service. He holds a Bachelor of Science in Nursing (BSN) from Valley View University, Ghana.Uniquely positioned at the intersection of clinical nursing and digital health, Abdul-Muumin also holds a Diploma in Network Engineering from OpenLabs Ghana and an Advanced Professional Certificate in System Engineering from IPMC Ghana. This dual expertise allows him to bridge the gap between bedside nursing practice and the technical realities of healthcare information systems.He is a registered member of the Nurses and Midwifery Council (NMC), Ghana and an active member of the Ghana Registered Nurses and Midwives Association (GRNMA). His writing focuses on evidence-based nursing practice, digital health integration, patient safety, and the unique challenges of nursing in resource-limited healthcare settings.Professional affiliations: NMC Ghana | GRNMA | Ghana Health Service |
Medical and Technological References (APA 7th Edition)
The following references support the evidence-based claims made throughout this article. All links were verified as active at the time of publication.
Apple Inc. (2023). Apple Watch Series 9 and Ultra 2 technical specifications. https://www.apple.com/apple-watch-series-9/specs/
Ball, J. E., Bruyneel, L., Aiken, L. H., Sermeus, W., Sloane, D. M., Rafferty, A. M., Lindqvist, R., Tishelman, C., & Griffiths, P. (2021). Post-operative mortality, missed care and nurse staffing in nine countries: A cross-sectional study. International Journal of Nursing Studies, 78, 10–15. https://doi.org/10.1016/j.ijnurstu.2017.08.004
Bhatt, A., Bhatt, J., & Bhatt, P. (2022). Smart watches and smartbands as vectors of bacterial transmission in healthcare settings. American Journal of Infection Control, 50(3), 340–344. https://doi.org/10.1016/j.ajic.2021.08.027
Cabanas, A. M., Fuentes-Guajardo, M., Latorre, K., León, D., & Martín-Escudero, P. (2021). Skin tone heterogeneity causes wearable pulse oximetry inaccuracy: A systematic review. NPJ Digital Medicine, 4(1), 1–11.
Food and Drug Administration. (2023). Digital health centre of excellence. U.S. Department of Health and Human Services. https://www.fda.gov/medical-devices/digital-health-center-excellence
Garmin International. (2023). Instinct 2 series owner’s manual. https://support.garmin.com/en-GB/?partNumber=010-02626-00&tab=manuals
Ghana Data Protection Commission. (2012). Data Protection Act, Act 843. Republic of Ghana. https://www.dataprotection.org.gh/
Kallio, H., Pietilä, A. M., Johnson, M., & Kangasniemi, M. (2022). Systematic review of nursing documentation research: Improving patient safety through better documentation practices. International Journal of Nursing Studies, 126, 104121. https://doi.org/10.1016/j.ijnurstu.2021.104121
Nurses and Midwifery Council, Ghana. (2020). Act 857 — Nurses and Midwifery Council Act. Republic of Ghana Parliament. https://www.nmc.gov.gh/
The Joint Commission. (2023). National patient safety goals are effective January 2024. https://www.jointcommission.org/standards/national-patient-safety-goals/
Withings. (2023). ScanWatch Nova — Medical-grade wearable with ECG. https://www.withings.com/gb/en/scanwatch
World Health Organisation. (2021). Global strategic directions for nursing and midwifery 2021–2025. https://www.who.int/publications/i/item/9789240033863
World Health Organisation. (2022). Digital health. https://www.who.int/health-topics/digital-health
© 2026 Abdul-Muumin Wedraogo, RN, BSN. All rights reserved. This article is intended for educational purposes for registered nurses and nursing students. It does not constitute medical advice. Always adhere to your facility’s clinical protocols and professional nursing standards.