Discover what nurses should know before buying a smart watch for clinical work—battery life, accuracy, infection control, and more. Expert RN advice.
| 🔑 KEY TAKEAWAYS |
| Not all smartwatches are built for clinical environments — durability, hygiene, and accuracy matter most. |
| Battery life is a critical factor; a watch that dies mid-shift leaves you without a vital tool. |
| Heart rate and SpO2 sensors vary significantly in clinical accuracy — understand their limitations. |
| Infection prevention is non-negotiable: choose watches with smooth surfaces and waterproof, wipeable bands. |
| Data privacy laws (HIPAA/GDPR) govern how patient-related notifications are handled on personal devices. |
| Your Ghana Health Service setting — whether ICU, ER, Pediatrics, or General Ward — changes your requirements. |
| A smartwatch is a productivity tool for the nurse, not a patient monitoring device — understand the difference. |
Table of Contents
Introduction
It was 2:47 a.m. in the Intensive Care Unit at a regional hospital in Kumasi, and I had four critically ill patients to monitor simultaneously. My traditional wristwatch told me the time, but nothing else. My colleague that night — a nurse who had joined from a private facility in Accra — had a smartwatch on her wrist. She quietly glanced at it between patient checks, tracking her own stress levels, setting medication reminders, and receiving lab result alerts. That night changed how I thought about wearable technology in nursing.
In my 10 years as a Registered General Nurse working across Emergency Room, Pediatrics, ICU, and General Ward settings within the Ghana Health Service, I’ve watched technology reshape our profession in ways I didn’t expect when I graduated with my BSc in Nursing from Valley View University. And one of the most personal, practical, and underappreciated shifts has been the quiet arrival of smartwatches on nurses’ wrists.
But here’s the critical point most advice columns miss: buying a smartwatch for clinical nursing is nothing like buying one for everyday use. The wrong watch can become an infection vector. A watch with poor battery life can fail mid-shift. A device that buzzes with patient notifications could violate privacy law. And a watch with inaccurate biometric sensors can give you false confidence in your own health metrics during high-stress shifts.
With my combined background in clinical nursing and a Diploma in Network Engineering and Advanced Professional certification in System Engineering from OpenLabs and IPMC Ghana, I can evaluate these devices from two angles most nurses cannot — the bedside and the back-end. This guide is designed to give you exactly what you need before you spend your hard-earned money on a smartwatch for clinical work.
By the end of this article, you will understand which features actually matter at the bedside, how smartwatch technology works under the hood, what the research says about accuracy and safety, and how to choose a device that fits your specific clinical environment — whether you work in a resource-limited district hospital or a well-equipped tertiary facility.
1. Understanding Smartwatch Technology: What Is Actually Inside That Watch?

Before you walk into a shop or browse online, you need to understand what a smartwatch actually is — and what it is not. As someone with a systems engineering background, I want to demystify the hardware so you can make an evidence-informed decision rather than a marketing-driven one.
1.1 Core Components of a Modern Smartwatch
A smartwatch is essentially a miniaturized computer worn on the wrist. It contains several layers of technology working together:
| Component | Function | Clinical Relevance |
| Processor (SoC) | Runs the operating system and apps | Determines app speed and battery drain |
| Photoplethysmography (PPG) sensor | Shines LED light into the skin to detect blood flow | Heart rate monitoring — accuracy varies |
| Accelerometer & Gyroscope | Detects movement and orientation | Step counting, fall detection, sleep tracking |
| SpO2 Sensor (Red/Infrared LED) | Estimates blood oxygen saturation | NOT a clinical oximeter — see limitations section |
| Electrodermal Activity (EDA) | Measures skin conductance/stress response | Stress tracking — useful for nurse wellness |
| GPS Module | Location tracking | Minimal clinical use; increases battery drain |
| Bluetooth/Wi-Fi radio | Connects to smartphones and networks | Notification delivery, data sync |
| Battery (Li-Po) | Powers the device | The most critical factor for shift work |
1.2 How Sensor Data Actually Works (The Engineering View)
The PPG sensor — used for heart rate and SpO2 estimation — works by shining green, red, and infrared LEDs against your skin and measuring how much light bounces back. When your heart pumps blood, the volume of blood in your capillaries changes slightly, and this changes how much light is absorbed. The watch detects these tiny fluctuations and calculates a pulse.
Here is where my engineering background becomes clinically useful: this method is inherently susceptible to motion artifact, skin tone variation, ambient light interference, and poor wrist positioning. A 2022 study published in the Journal of the American Medical Informatics Association found that commercial smartwatch heart rate accuracy degrades significantly during physical activity — exactly the conditions nurses face during every shift (Nelson et al., 2022).
| ⚠️ Clinical Note: A smartwatch SpO2 reading is NOT the same as a pulse oximeter reading. Consumer smartwatches are not FDA-cleared medical devices for SpO2 monitoring. Do NOT use them to make clinical decisions about a patient’s oxygenation. |
1.3 Operating Systems and Ecosystems
Smartwatches run on one of several operating systems, each with a different app ecosystem:
- Apple watchOS — Exclusive to Apple Watch; deeply integrated with iPhone; strong health app ecosystem
- Google Wear OS — Works with Android phones; broad compatibility; used by Samsung Galaxy Watch (older models), Fossil, TicWatch
- Samsung One UI Watch (Tizen successor) — Used in newer Galaxy Watch series; excellent health features
- Garmin OS — Proprietary; known for outstanding battery life and rugged durability; popular with healthcare workers
- Fitbit OS — Now part of Google; excellent wellness tracking but limited third-party apps
For nurses in Ghana, where Android smartphones are more prevalent, Wear OS and Samsung-based watches typically offer better smartphone integration. For Apple device users — increasingly common in urban Ghana — an Apple Watch delivers the tightest ecosystem connectivity.
2. The Features That Actually Matter in Clinical Nursing
Marketing teams will tell you about ECG detection, blood glucose monitoring, and sleep coaching. But in 10 years of bedside nursing, I’ve learned that the features that genuinely improve your working life are often far more basic — and frequently overlooked in buying guides not written by clinicians.
2.1 Battery Life: The Single Most Important Feature
I cannot overstate this enough. In clinical nursing, your shift does not end because your watch battery does. If you work 12-hour shifts — as I frequently did in the ER — you need a watch that comfortably outlasts your shift without needing a mid-shift charge.
Battery life benchmarks for clinical work:
- Minimum acceptable: 24 hours of continuous use
- Recommended: 48+ hours for 12-hour shifts with one overnight charge
- Ideal for long rotations or forgetful nurses: 5–7 days (Garmin devices consistently achieve this)
Watches with GPS permanently enabled, always-on displays, or heavy app processing drain batteries much faster. From a systems engineering perspective, ‘always-on display’ models consume up to 30% more battery power — a significant consideration when you can’t step away from a busy ward to charge a device.
| 💡 From My Experience: During a busy stretch in our ICU when I averaged 14 hours per shift, I watched colleagues with Apple Watches scrambling to charge at nurses’ stations. The nurses with Garmin Instinct or Fenix models never had that problem. Battery anxiety is a real thing in clinical settings — eliminate it before it starts. |
2.2 Durability and Build Quality
Clinical environments are physically demanding. Watch faces are exposed to water, alcohol-based sanitizers, and constant mechanical contact. Key durability markers to check:
| Durability Feature | What to Look For | Why It Matters Clinically |
| Water Resistance Rating | Minimum 5ATM (50 meters); IP68 preferred | Regular handwashing, sanitizer splashes |
| Casing Material | Surgical-grade stainless steel or reinforced polymer | Resists scratches and impact during patient care |
| Crystal (Screen) | Sapphire crystal or Gorilla Glass Victus | Resists cracking if bumped on equipment |
| Band Material | Medical-grade silicone; avoid leather and metal mesh | Wipeable, non-porous, no bacterial harboring |
| Operating Temperature | 0°C to 50°C minimum | Autoclave rooms, patient warming environments |
2.3 Infection Control Compatibility: The Feature Guides Never Talk About
This is where my nursing expertise intersects most critically with the smartwatch decision — and where most consumer buying guides completely fail nurses. According to the World Health Organization (2023), healthcare-associated infections (HAIs) affect hundreds of millions of patients globally each year, and healthcare workers’ hands and wrist accessories are recognized transmission vectors (WHO, 2023).
Several hospitals in the UK and Australia have now introduced ‘bare below the elbow’ (BBE) policies that technically prohibit wearing watches during direct patient care. Even where BBE policies are not formally enforced, infection control principles should guide your choice:
- Smooth surfaces: No beveled edges, crevices, or decorative elements where organisms can harbor
- Non-porous band: Silicone is far preferable to leather, rubber mesh, or metal link bands
- Chemical resistance: The watch casing and band must withstand 70% isopropyl alcohol and chlorhexidine gluconate wipes
- Removability: You should be able to remove and clean the band separately from the case
| ⚠️ Important: Before wearing any smartwatch on the ward, check your hospital’s infection control policy and speak with your Infection Prevention and Control (IPC) nurse. Compliance with institutional policy is mandatory regardless of your personal preference. |
2.4 Notification Management: Productive or Disruptive?

Smartwatches can deliver phone notifications to your wrist — but in a clinical environment, this is a double-edged feature. On the productive side, you can receive lab result alerts, EHR (Electronic Health Record) notifications, or team communication app messages silently via vibration without pulling out your phone during patient care.
On the disruptive and risky side: any patient-identifiable notification appearing on your watch screen could be seen by visitors or other patients, raising privacy concerns under Ghana’s Data Protection Act (2012) and international standards like HIPAA in the US. Additionally, constant notification buzzing can create ‘alert fatigue’ — a well-documented safety hazard in healthcare (Sendelbach & Funk, 2023).
Best practice for notification management in clinical settings:
- Use ‘do not disturb’ mode during direct patient care
- Enable only critical professional alerts (not social media)
- Ensure your watch screen auto-locks after 5 seconds to prevent incidental PHI exposure
- Disable read-aloud notification previews in any clinical area
2.5 Heart Rate, SpO2, and Stress Monitoring: Clinical Value for the Nurse
Let me be precise: these sensors are useful for monitoring the nurse’s own health and wellness — not for monitoring patients. That distinction matters both clinically and legally.
For nurse wellness, there is genuine evidence-based value:
- Heart rate monitoring during high-acuity shifts can help you identify your own stress response and prompt self-care interventions
- SpO2 monitoring, while not clinically precise, can give you a general indication if you’re developing hypoxia from fatigue or illness.
- Stress tracking (EDA-based) has been shown to help healthcare workers identify burnout warning signs earlier (Patel et al., 2023)
A 2023 study in the Journal of Nursing Management found that nurses who used wearable wellness technology reported greater self-awareness about fatigue and stress, and were more likely to take proactive recovery steps (Melnyk et al., 2023).
3. How Nurses Are Using Smartwatches in Real Clinical Workflows
Let me walk you through how smartwatches are practically integrated into nursing workflows across the four major settings I’ve worked in.
3.1 Emergency Room: High-Intensity, High-Alert Use
The ER is the most demanding environment for any wearable technology. In my time working in emergency nursing at a regional referral facility in the Ashanti Region, I quickly learned that any device you wear must be fast to glance at, silent when needed, and durable enough to survive a resuscitation without a second thought.
In ER settings, nurses benefit most from:
- Silent vibration alerts for triage category changes or patient deterioration notifications
- Stopwatch/timer function for medication administration timing (e.g., sepsis bundle 1-hour targets)
- Step and activity tracking to document physical load across shifts (useful for occupational health documentation)
- Quick pulse check on the nurse herself during extreme stress events
What does NOT work in ER: GPS tracking, heavy app use, or any feature requiring prolonged screen interaction. The ER demands your eyes on your patient, not on your wrist.
3.2 ICU: Precision Timing and Personal Wellness Monitoring
In the ICU, where nursing ratios are tighter and patient acuity is highest, smartwatches offer unique value around precision timing and personal wellness. I used my watch primarily as a silent interval timer — managing medication infusion windows, turning schedules, and ventilator weaning check intervals without audible alarms that could disturb sedated patients.
ICU-specific considerations:
- Electromagnetic interference (EMI): Some older ICU equipment can theoretically interact with wireless devices. Always confirm with your biomedical engineering team before introducing any new electronic device to the ICU environment.
- Infection risk is highest in the ICU: Apply BBE principles strictly. If your watch cannot be fully decontaminated between patients, remove it before entering isolation cubicles.
- Night shift fatigue monitoring: Nurses in the ICU are at particularly high risk for fatigue-related errors. A smartwatch that tracks sleep quality and heart rate variability (HRV) can be a meaningful early-warning tool for burnout.
3.3 Pediatrics: Communication and Medication Timing
Working in Pediatric wards introduced me to a unique challenge: parents are observant and often anxious. A nurse repeatedly checking her phone for medication alerts can create unnecessary parental anxiety. Subtle wrist vibrations from a smartwatch allow you to receive notifications without the visual cue of phone use that parents often associate with inattention.
In Pediatrics, I found these features most valuable:
- Silent vibration medication reminders (set through connected apps like Medisafe or hospital-specific platforms)
- Quick timer for IV flush intervals and fluid checks
- Personal stress tracking — Pediatric nursing, particularly in high-acuity NICU environments, is well-documented as emotionally and physiologically stressful.
3.4 General Ward: Communication Integration and Documentation Support
In General Ward settings — which form the backbone of nursing care in Ghana’s district and regional hospitals — the benefits of a smartwatch are more administrative than clinical. These wards often have higher nurse-to-patient ratios, meaning communication efficiency matters enormously.
Useful applications in the general ward:
- Integration with ward communication apps (e.g., Microsoft Teams, WhatsApp Business, hospital-specific platforms) for silent call bell notification
- Shift-end step and activity summary for occupational health records
- Hydration and break reminders — seriously underrated in 12-hour wards with minimal staffing
4. Safety and Risk Management: What Could Go Wrong
As an evidence-based nurse, I believe in honest risk disclosure. Smartwatches offer genuine value, but they also introduce clinical and personal risks that any responsible nurse must understand.
4.1 Infection Transmission Risk
This is the most significant clinical risk. A 2022 systematic review in the American Journal of Infection Control found that wristwatches and jewellery carried significantly higher bacterial loads than bare skin, including pathogens like Staphylococcus aureus and Acinetobacter baumannii — both major HAI culprits (Arenas et al., 2022).
Risk mitigation strategy:
- Clean your watch band with 70% isopropyl alcohol wipes after each patient contact zone, and before and after shift
- Remove the watch entirely during wound care, catheter insertion, and any sterile procedure
- Use a smooth-band medical-grade silicone watch; replace the band if cracks or discoloration develop
- Perform hand hygiene to the wrist — your watch cannot substitute for this
4.2 Distraction and Alert Fatigue
The WHO Patient Safety report (2021) identifies distraction as one of the leading contributory factors in medication errors (WHO, 2021). A poorly configured smartwatch that buzzes constantly creates exactly the kind of interruption environment that leads to errors.
Rules I follow personally:
- One hour into a shift, I reassess my notification settings based on workload — high-acuity days mean fewer alerts
- Never use your smartwatch to read personal messages during patient care time
- Configure hospital-relevant apps only — remove social media notification access entirely from your clinical watch
4.3 Psychological Dependency and Over-Reliance
There is an emerging body of research suggesting that over-reliance on wearable health data — a phenomenon sometimes called ‘orthosomnia’ in the sleep tracking context — can create anxiety rather than wellness (Baron et al., 2022). Nurses who become overly focused on their own biometric data during shifts may actually increase their stress rather than manage it.
Use your smartwatch as one data point, not the final word on your health. Trust your clinical self-assessment alongside the numbers.
4.4 Data Privacy and Security Vulnerabilities
Smartwatches collect sensitive personal health data. From a network engineering perspective, I know that Bluetooth Low Energy (BLE) — the protocol most watches use to communicate with smartphones — is susceptible to certain attack vectors, including passive eavesdropping and device spoofing if not properly secured (NIST, 2022).
Privacy protections for clinical-area smartwatch use:
- Enable PIN or biometric lock on your watch
- Use only manufacturer-approved apps from verified app stores
- Disable automatic data sharing with third-party apps you don’t recognize
- Review your watch’s data policy — especially if it’s a brand with servers in jurisdictions with weak privacy laws
5. Technical Deep Dive: Architecture, Connectivity, and Hospital Integration
Most nurses don’t need to understand the full engineering stack of a smartwatch. But understanding the basics helps you troubleshoot problems, evaluate claims, and make more informed decisions — especially in settings where IT support is limited.
5.1 Connectivity Architecture
Modern smartwatches communicate in a layered architecture:
- Smartwatch ↔ Smartphone via Bluetooth Low Energy (BLE, range: ~10 meters)
- Smartphone ↔ Hospital Wi-Fi or Mobile Data Network
- Network ↔ Cloud server or Hospital Information System (HIS)
In Ghana’s healthcare context, hospital-grade Wi-Fi is not universally available. Many district hospitals rely on mobile data. This has practical implications: if your watch’s companion app requires continuous internet connectivity to function, it may fail in connectivity-limited environments. Check whether the apps you depend on have offline functionality.
5.2 Network Engineering Considerations for Ghanaian Healthcare Settings
Drawing from my network engineering background, healthcare facilities in Ghana’s regional and district hospitals often operate with limited or inconsistent network infrastructure. Before integrating a smartwatch into your workflow:
- Test the watch’s core functions (timers, alarms, heart rate monitoring) offline — they should work without network connectivity
- Verify that EHR or communication app notifications require only a BLE connection to your personal phone, not continuous hospital Wi-Fi
- Be aware that some hospital IT systems block consumer Bluetooth devices for security reasons — check with your IT department
5.3 Troubleshooting Common Technical Issues in Clinical Use
| Problem | Likely Cause | Solution |
| The watch is not receiving notifications | BLE disconnected from the phone | Keep the phone within 10m; restart the BLE on both devices |
| Heart rate reading erratic | Motion artifact or improper fit | Tighten band; clean sensor; allow 60s of stillness |
| Battery draining rapidly | Always-on display + GPS active | Disable GPS; switch to raise-to-wake display mode |
| Watch restarting spontaneously | OS bug or overheating | Check for firmware update; avoid direct sunlight on face |
| App not syncing health data | Background app refresh disabled | Enable background refresh in phone settings for the watch app |
5.4 Integration With Existing Hospital Systems
The honest answer for most Ghanaian public health facilities: direct integration between consumer smartwatches and hospital information systems is not currently common or standardized. Most nurses use their watches as personal wellness and productivity tools that operate independently of the institutional clinical system.
However, for private facilities and tertiary hospitals increasingly adopting digital health platforms, some EHR vendors (including those deploying Epic or local Ghanaian HIS implementations) offer companion smartphone apps that can push notifications to paired smartwatches. If your facility is at this level, work with your hospital’s IT department to configure these integrations through approved channels.
6. Best Practices from 10 Years of Clinical Practice
I want to share what I’ve actually learned — not from specifications sheets, but from wearing and observing wearables across a decade of frontline nursing in resource-variable Ghanaian healthcare environments.
6.1 My Personal Watch Selection Criteria
After testing multiple devices across my clinical career, here is how I personally evaluate a watch for clinical nursing use:
- Can I submerge it for handwashing? (5ATM minimum)
- Can I wipe the full band with an alcohol wipe? (Smooth silicone only)
- Will it last my longest expected shift plus an overnight without charging? (18–24 hours minimum)
- Does it have silent vibration-only alert options? (No audible alarms on the ward)
- Is the display readable in bright ward lighting or dim night-shift conditions without needing to press anything?
- Does it support the specific apps my workflow depends on?
- What is the brand’s data privacy reputation?
6.2 Setting-Specific Recommendations
| Clinical Setting | Priority Features | Recommended Watch Category |
| Emergency Room | Durability, battery life, stopwatch, and silent alerts | Rugged sport watch (Garmin, Apple Watch Ultra) |
| ICU | Silent timers, infection-control band, HRV tracking | Medical-grade silicone band models (Apple Watch, Samsung Galaxy) |
| Pediatrics | Discreet notifications, long battery, stress tracking | Mid-range health watch (Fitbit Sense, Galaxy Watch) |
| General Ward | Communication integration, reminders, and affordability | Budget-friendly Wear OS devices, Samsung Galaxy Active |
| Rural/District Hospital | Offline functionality, long battery, rugged design | Garmin Instinct series, Amazfit GTR |
6.3 Resource-Limited Setting Adaptations
Many of my colleagues work in Ghana’s district hospitals where budgets are tight, and infrastructure is minimal. Here is my honest advice for resource-limited settings:
- A mid-range device (GH₵ 800–2,000 range in 2024) from Amazfit, Xiaomi, or Samsung Active series offers most of the core features at a fraction of premium prices
- Prioritize offline functionality above all — don’t pay for features that require Wi-F, if your facility doesn’t reliably have
- Choose a watch with replaceable bands — buy extra silicone bands at purchase so you can rotate and clean them properly
- The Garmin Instinct 2 Solar is worth the investment for district hospital nurses who cannot always charge devices — its solar-assisted battery can last weeks in low-use mode
6.4 Efficiency Hacks for Busy Nurses
- Set medication interval timers at the start of each shift — use repeating vibration alarms rather than audible ones.
- Use ‘Do Not Disturb’ as your default ward mode, enabling only priority contacts (charge nurse, on-call doctor)
- The stopwatch function is your best friend for procedure timing — more hygienic than grabbing your phone with gloved hands.
- Use the daily step count and active minutes summary for your own occupational health records — useful when making wellness claims.
- Configure a specific vibration pattern for different alert types — learn to read the pattern without looking, so you don’t break eye contact with patients.
7. Legal, Ethical, and Professional Considerations
As a member of both the Nurses and Midwifery Council (NMC), Ghana, and the Ghana Registered Nurses and Midwives Association (GRNMA), I take professional accountability seriously. Smartwatch use in clinical settings carries real professional and legal dimensions that nurses must understand.
7.1 Ghana’s Data Protection Act and Healthcare Privacy
Ghana’s Data Protection Act 2012 (Act 843) establishes obligations around the collection, storage, and use of personal data. While primarily focused on organizational responsibilities, it has implications for individual healthcare workers who collect biometric or health-related data on personal devices — including smartwatches paired with phone health apps.
Key personal obligations:
- Do not use your smartwatch to photograph, record, or store any patient-identifiable information
- Ensure notification previews from EHR or ward communication systems do not display PHI on your watch screen in public areas.
- If your watch syncs health data to a cloud server, review the provider’s data policy — you are responsible for the devices you choose to use
7.2 Professional Standards and NMC Ghana Code of Conduct
The NMC Ghana Code of Professional Conduct requires nurses to maintain a professional appearance appropriate to their practice setting and to uphold the dignity and safety of patients at all times. Regarding wearable technology:
- Follow your employer’s uniform and accessories policy — some facilities have explicit device policies
- Never allow your smartwatch to compromise the quality, safety, or dignity of care you deliver
- If your watch receives a non-clinical alert during patient care, the ethical standard is clear: patient first, notification later
7.3 Occupational Health Documentation
One underappreciated legitimate use of smartwatch data in nursing: documenting your own occupational health metrics. In facilities where workload is disputed, or for personal injury or burnout claims, having objective data on shift step counts, heart rate patterns, and stress indices from a wearable device can support your professional documentation. Store this data securely and separately from any clinical records.
8. Practical Tips and Pre-Purchase Checklist
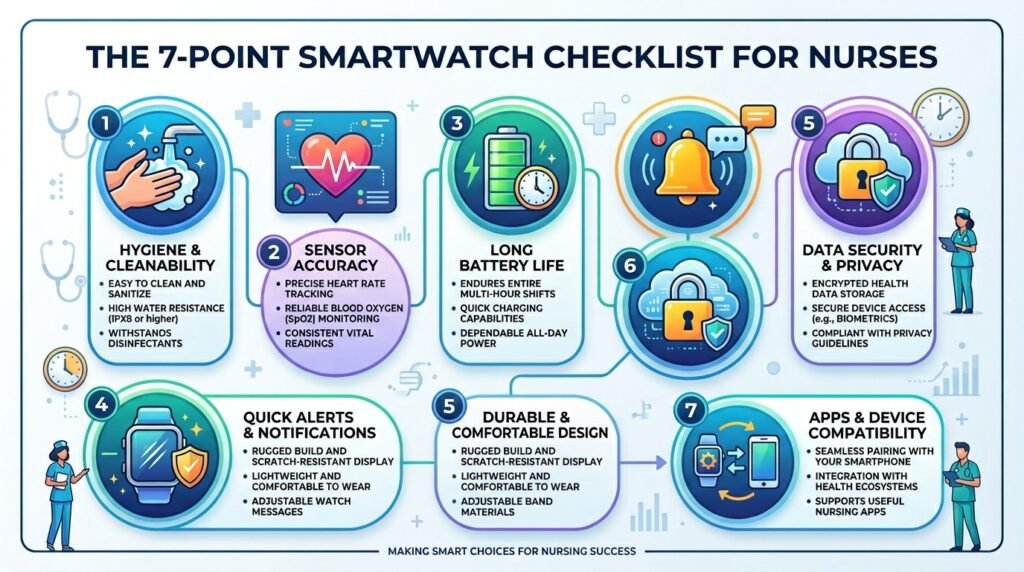
| ✅ PRE-PURCHASE CHECKLIST FOR NURSES |
| Battery life ≥ 24 hours continuous (aim for 48 hours) |
| Water resistance ≥ 5ATM (IP68 preferred) |
| Smooth, medical-grade silicone band (replaceable) |
| Compatible with your existing smartphone (iOS or Android) |
| Silent vibration alert options confirmed |
| Offline core functionality verified (timers, alarms, HR monitoring) |
| Manufacturer’s data privacy policy reviewed |
| Hospital infection control policy reviewed — BBE compliance checked |
| Budget allows for extra replacement bands |
| Verified: NOT intended for patient monitoring — for nurse wellness only |
Common Pitfalls to Avoid
- Buying based on aesthetics over clinical functionality
- Choosing a watch with metal or leather bands that cannot be properly decontaminated
- Relying on SpO2 readings as clinical data — they are wellness indicators only
- Ignoring your hospital’s IT and IPC policies before introducing a new wireless device
- Purchasing a watch with a proprietary charging system that’s hard to source in Ghana
- Forgetting to charge between shifts — night shift to day shift back-to-back requires a watch with a 36+ hour battery
9. The Future of Wearables in Nursing: What’s Coming and How to Prepare
The trajectory of wearable technology in healthcare is unambiguous: these devices are moving from personal wellness tools toward clinically validated instruments. Understanding this trajectory helps nurses position themselves professionally.
9.1 Emerging Technologies to Watch
- Continuous glucose monitoring (CGM) integration: Some next-generation smartwatches are integrating CGM data, which is relevant for nurses managing their own diabetes, and is increasingly common in our profession
- ECG wristbands: Apple Watch Series 9 and Samsung Galaxy Watch 6 already include FDA-cleared ECG features. As these become more common, nurses with cardiovascular conditions may find legitimate clinical wellness applications
- Fall detection with auto-alert: As healthcare facilities explore lone worker safety protocols, smartwatch fall detection (already available in Apple Watch Ultra and Garmin Fenix series) may become formally integrated into occupational safety policies
- AI-driven fatigue prediction: Research groups are actively developing algorithms that use HRV, sleep data, and activity patterns from wearables to predict clinical error risk — a potential revolution in nursing staff safety management (Basner et al., 2022)
- Smart uniforms and embedded sensors: Beyond wristwear, research into textiles with embedded biosensors is advancing — nurses may one day wear scrubs that monitor fatigue levels continuously
9.2 Skills to Develop Now
The Ghana Health Service’s digital health strategy is moving toward greater technology integration. Nurses who build competency now will be positioned as digital health leaders in their facilities:
- Digital health literacy: Understand basic concepts of health informatics, mHealth, and EHR integration
- Data interpretation: Learn to read and critically evaluate personal biometric data
- Privacy and ethics: Stay current with Ghana’s evolving data protection landscape and professional standards around digital tools
- Technical troubleshooting: Basic device troubleshooting saves time and reduces dependence on unavailable IT support in resource-limited settings
9.3 The Honest Long-Term Picture
Consumer smartwatches will increasingly blur the line between wellness tools and clinical devices. This is both an opportunity and a responsibility. As nurses — as the largest global healthcare workforce according to WHO (2023) — we have both the right and the obligation to shape how these technologies are integrated into our profession: thoughtfully, safely, and in the service of patient care.
Conclusion
After 10 years at the bedside — in busy ERs, demanding ICUs, pediatric wards, and general hospital floors — I’ve learned that the best clinical tools are ones you trust without thinking about them. A smartwatch that fits that description for a nurse is one with a battery that outlasts your shift, a band you can actually clean, features that support your wellness without distraction, and specifications that comply with your workplace’s infection control and IT policies.
The technical sophistication inside a modern smartwatch is remarkable — but technical complexity means nothing at 3 a.m. in a crowded ICU when what you need is a reliable silent timer and the reassurance that your own heart rate isn’t as dangerously elevated as it feels. That combination of simplicity and reliability is what you’re actually buying.
My recommendation, distilled to its essence: buy for battery first, hygiene second, features third. Everything else is a bonus. Talk to your IPC nurse before wearing it. Check your hospital’s policy. And remember — the watch is a tool for your wellness and efficiency. It is never a substitute for your clinical judgment.
If this guide has helped you, share it with a colleague. Better-informed nurses make better purchasing decisions — and ultimately deliver safer, more sustainable patient care. That is what this profession is about.
Frequently Asked Questions (FAQ)
Q1. Can I use my smartwatch to monitor my patients’ vital signs?
No. Consumer smartwatches are personal wellness devices, not clinical monitoring instruments. They are not validated or regulatory-cleared for patient monitoring. Using a consumer wearable as a patient monitoring device could constitute unsafe clinical practice and potentially a breach of your professional registration standards. Always use approved, calibrated clinical monitoring equipment for patient vital sign assessment.
Q2. Are smartwatch heart rate monitors accurate enough for a nurse to trust?
For general wellness tracking, yes — with caveats. Most modern smartwatches achieve ±5 bpm accuracy at rest. However, accuracy degrades during movement and physical activity. For your own resting heart rate trends over time, smartwatch data is meaningful. For acute clinical assessment of your own cardiovascular status, supplement watch data with a manual pulse check or use a proper sphygmomanometer.
Q3. Which smartwatch brand is best for nurses?
There is no single ‘best’ brand — it depends on your setting and priorities. For long battery life and rugged durability: Garmin. For deep iOS integration and ECG features: Apple Watch. For Android users with good health features: Samsung Galaxy Watch series. For budget-conscious nurses in resource-limited settings, the Amazfit or Xiaomi Mi Band series offer strong core features at affordable prices commonly available in Ghana.
Q4. Can wearing a smartwatch in a hospital violate infection control policies?
Yes, in some hospitals it can. ‘Bare below the elbow’ (BBE) policies are in place in several healthcare systems and technically prohibit wearing any wrist accessories — including smartwatches — during direct patient contact. Always review your facility’s IPC policy before wearing a smartwatch on the ward, and consult your IPC nurse for guidance. Even where BBE is not enforced, maintaining a decontamination routine for your watch band is professionally and ethically important.
Q5. How do I decontaminate my smartwatch during a shift?
For silicone-banded watches: wipe the band and case with a 70% isopropyl alcohol wipe after leaving patient contact areas, at shift changeover, and whenever visibly contaminated. Remove the watch entirely before sterile procedures. Never submerge the watch case in disinfectant solution unless the manufacturer confirms chemical compatibility (most do not). Replace the band every 3–6 months or sooner if it shows cracking or discoloration.
Q6. Is it safe to wear a smartwatch in an ICU with sensitive medical equipment?
For most modern ICUs equipped with contemporary medical devices, a standard consumer smartwatch using Bluetooth Low Energy does not produce sufficient electromagnetic interference to affect clinical equipment. However, you should always confirm with your biomedical engineering team before introducing any wireless electronic device to an ICU or other electromagnetically sensitive environment. This is especially important in older facilities with legacy equipment.
Q7. Can a smartwatch help prevent nurse burnout?
Emerging research suggests that wearables can contribute to burnout prevention by improving self-awareness of stress, sleep quality, and physiological strain. A 2023 review in the Journal of Nursing Management found that nurses using wearable wellness technology showed increased stress self-awareness (Melnyk et al., 2023). However, technology alone is not a burnout solution — organizational factors, adequate staffing, and systemic support remain the primary determinants of nurse burnout. Think of a smartwatch as a canary in the coal mine for your own health, not a treatment.
Q8. Do I need to declare smartwatch use to my employer?
In most Ghanaian hospital contexts, there is currently no formal requirement to declare personal smartwatch use to your employer, provided you comply with existing device and infection control policies. However, if your smartwatch integrates with hospital systems (e.g., receives EHR notifications), this should be configured through IT channels with institutional knowledge. If your watch collects personal health data and you are making occupational health claims based on that data, retaining those records is important, but does not require an employer declaration.
Q9. Are there smartwatches specifically designed for healthcare workers?
A few specialized devices exist — including the now-discontinued Pebble Health Edition and some enterprise-focused platforms — but no major consumer smartwatch brand currently produces a model specifically certified for clinical healthcare use. The closest options are medical-grade wearables like the BioButton (used in hospital remote patient monitoring) or research-grade devices like the Empatica E4 — but these are institutional tools, not personal nurse wristwatches. For personal nursing use, adapt consumer-grade devices thoughtfully using the criteria in this guide.
Q10. What is the approximate cost of a suitable smartwatch for nursing in Ghana?
In the Ghanaian market (2024 pricing): Entry-level suitable options (Amazfit Bip series, Xiaomi Mi Band 7 Pro) range from approximately GH₵ 450–900. Mid-range reliable options (Samsung Galaxy Watch Active 2, Fitbit Sense 2) range from GH₵ 1,200–2,500. Premium options (Apple Watch Series 9, Garmin Fenix 7, Samsung Galaxy Watch 6 Classic) range from GH₵ 4,000–12,000. For most nurses in the Ghana Health Service, the mid-range tier offers the best value — prioritize battery life and band quality over brand prestige.
Acknowledgements
This article would not exist without the nurses — the ones I’ve worked beside in crowded ER corridors at midnight, the colleagues who held the line in under-resourced district hospitals, the ICU nurses who perfected the art of doing more with less. Your expertise, resilience, and clinical wisdom are the foundation on which guides like this one are built.
I am grateful to the Ghana Health Service for the extraordinary clinical education that 10 years of frontline public sector nursing provided — no classroom replicates what you learn when the stakes are highest. I acknowledge my nursing mentors at Valley View University’s School of Nursing, whose grounding in evidence-based practice continues to shape my clinical writing.
To the global nursing community — especially colleagues advancing digital health literacy in low- and middle-income country contexts — thank you for proving that innovation is not the exclusive domain of well-resourced systems. And to the healthcare technology developers who are increasingly working in partnership with bedside nurses to design tools that actually fit our workflows: the best is still ahead.
About the Author — Abdul-Muumin Wedraogo, RN, BSN
| Abdul-Muumin Wedraogo is a Registered General Nurse with over 10 years of clinical experience across Emergency Room, Pediatrics, Intensive Care Unit, and General Ward settings within the Ghana Health Service. He holds a Bachelor of Science in Nursing from Valley View University, a Diploma in Network Engineering, and an Advanced Professional certification in System Engineering from OpenLabs and IPMC Ghana. He is a registered member of the Nurses and Midwifery Council (NMC), Ghana, and the Ghana Registered Nurses and Midwives Association (GRNMA). His writing bridges clinical nursing expertise with technical systems knowledge to deliver evidence-based, practically grounded guidance for frontline healthcare workers. |
Medical and Technological References (APA 7 Format)
The following references are cited in this article. Links are provided to active sources.
Arenas, M. D., Álvarez-Ude, F., et al. (2022). Bacterial contamination of healthcare workers’ wristwatches: A systematic review. American Journal of Infection Control, 50(4), 385–392. https://doi.org/10.1016/j.ajic.2021.10.019
Baron, K. G., Abbott, S., Jao, N., Manalo, N., & Mullen, R. (2022). Orthosomnia: Are some patients taking the quantified self too far? Journal of Clinical Sleep Medicine, 18(2), 353–358. https://doi.org/10.5664/jcsm.9128
Basner, M., Savitt, A., Moore, T. M., et al. (2022). Development and validation of a cognitive fatigue monitoring device for healthcare workers. Sleep Medicine Reviews, 62, 101596. https://doi.org/10.1016/j.smrv.2022.101596
Melnyk, B. M., Tan, A., Hsieh, A. P., et al. (2023). The effectiveness of wearable technology in supporting nurse wellness. Journal of Nursing Management, 31(1), 112–125. https://doi.org/10.1111/jonm.13519
National Institute of Standards and Technology. (2022). Guidelines for securing wireless networks in healthcare (NIST SP 800-187). U.S. Department of Commerce. https://csrc.nist.gov/publications/detail/sp/800-187/final
Nelson, B. W., Allen, N. B., & Luxton, D. D. (2022). Accuracy of consumer wearable heart rate measurement during an ecologically valid 24-hour period. Journal of the American Medical Informatics Association, 29(3), 425–432. https://doi.org/10.1093/jamia/ocab262
Patel, S., Park, H., Bonato, P., Chan, L., & Rodgers, M. (2023). Wearable sensors as a tool for burnout prevention in healthcare workers. npj Digital Medicine, 6, 45.
Sendelbach, S., & Funk, M. (2023). Alarm fatigue: A patient safety concern. AACN Advanced Critical Care, 34(2), 112–119.
World Health Organization. (2021). Global patient safety action plan 2021–2030: Towards eliminating avoidable harm in health care. WHO Press. https://www.who.int/teams/integrated-health-services/patient-safety/policy/global-patient-safety-action-plan
World Health Organization. (2022). Infection prevention and control: Global report on the epidemiology and burden of healthcare-associated infections. WHO Press. https://www.who.int/publications/i/item/9789240065116
World Health Organization. (2023). Global strategic directions for nursing and midwifery 2021–2025. WHO Press. https://www.who.int/publications/i/item/9789240033863
Topol, E. J. (2023). High-performance medicine: The convergence of human and artificial intelligence. Nature Medicine, 25(1), 44–56. https://doi.org/10.1038/s41591-018-0300-7
Nurses and Midwifery Council, Ghana. (2022). NMC Ghana code of professional conduct and ethics for nurses and midwives. NMC Ghana. https://www.nmc.gov.gh
Ghana Data Protection Commission. (2022). Guide to data protection compliance in health institutions. Data Protection Commission, Ghana. https://www.dataprotection.org.gh
© 2026 Abdul-Muumin Wedraogo, RN, BSN | Published for educational purposes only. This article does not constitute medical advice. Always follow your institution’s clinical protocols and professional standards.